| visit: www.infertilitytutorials.com |
|
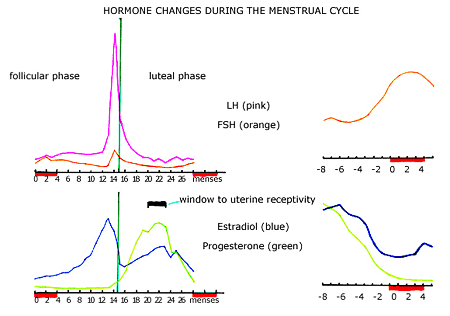
In a natural (spontaneous) menstrual cycle there is a precisely coordinated sequence of hormone changes that allow for the maturation and ovulation of one mature egg. Immediately prior to the onset of menses, FSH concentration rises to initiate the rapid development of several follicles (each of which has been prepared for that particular menstrual cycle over a several month timeframe). As these follicles develop, one of the racing follicles is normally chosen as the follicle destined to become the dominant follicle (the follicle that will ovulate). This dominant follicle develops an enhanced local blood supply (to receive a greater percentage of the circulating FSH) and a greater number of specific FSH receptors (to bind more of the circulating FSH). Overall, the circulating FSH concentration declines during most of the follicular (pre ovulatory) phase of the menstrual cycle, which leads to degeneration of all but the dominant follicle. Estradiol is the most bioactive form of estrogen. The circulating concentration of estradiol rises dramatically during the follicular phase of the menstrual cycle, which promotes growth of the endometrial lining of the uterus (uterine cavity). At a certain point in the menstrual cycle the LH surge occurs to trigger ovulation. It is currently thought that the ovary essentially tells the pituitary gland that it has an egg that is mature and ready to ovulate, and that the ovary does this somehow by means of the elevated circulating estradiol concentration. Once the LH surge has been initiated (to trigger ovulation), the estradiol concentration drops (prior to the release of the mature egg or ovulation). There is a second more subtle increase in estradiol concentration during the luteal phase of the menstrual cycle. The LH concentrations during the follicular phase of the menstrual cycle are pulsatile and generally low. About 36 hours prior to ovulation, a sudden rapid elevation in LH concentration (known as the LH surge) is initiated. This LH surge triggers the final maturation of the egg and the steps within the ovary that are required for release of the egg (ovulation). Progesterone concentration begins to rise (subtly) with the LH surge immediately prior to ovulation. The bulk of the increase in progesterone concentration occurs following ovulation. Several days following ovulation, the uterine endometrial lining becomes receptive to an implanting embryo (the window of uterine receptivity) for just a few days. Progesterone production within the ovary is supported by pituitary LH for about 14 days and if the woman becomes pregnant then continued ovarian progesterone production is supported by hCG (a hormone produced by some of the placental cells of the growing pregnancy, often called the pregnancy hormone). If the woman does not become pregnant, the progesterone and estrogen concentrations drop and the endometrial lining (that was developed) is shed as the menstrual flow. Graphs are based upon data collected by Dr. Samuel S.C. Yen. | |||||||||||||||