| visit: www.infertilitytutorials.com |
|
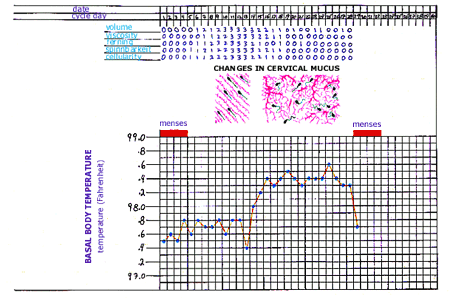
Cervical Mucus
The uterine cervix (opening or mouth of the uterus) normally extends into the vaginal canal near the top (innermost portion) of the vagina. Therefore, the cervix can be positioned several inches from the outer opening of the vaginal vault. The cervix can usually be seen clearly using a vaginal speculum during a gynecologic exam, at which time cervical mucus can be removed selectively from the cervical canal. Women who attempt to remove their own cervical mucus by means of a digital (finger) exam often are not able to obtain freshly produced cervical mucus. Therefore women who check their own cervical mucus may be misled since they may be viewing mucus from within the vagina that is several days old. Cervical mucus is a highly complex secretion that is continuously produced by the secretory cells of the cervix. Changes in the physical properties of cervical mucus during a normal spontaneous menstrual cycle have been described for over 25 years. Dr. Kamran S. Moghissi was one of the pioneers in the field of cervical mucus research and his postcoital test includes assessment of five physical characteristics (variables) of the mucus. Just prior to ovulation the cervical mucus should obtain the highest overall mucus score (using this test). The variables used (by Dr. Moghissi) to assess cervical mucus are (1) amount (cervical mucus is aspirated from the cervical canal under direct visualization using a syringe or other instrument), (2) spinnbarkeit (mucus is placed on a microscope slide, covered with a cover slip, the cover slip is drawn away from the slide, the length of the mucus thread that is created between the coverslip and slide just before breaking is measured in centimeters as the spinnbarkeit), (3) ferning (mucus that has been spread on a microscope slide is allowed to dry and the degree of crystal formation (ferning) is assessed using a microscope), (4) viscosity (the quality of a substance that displays a resistance to flow or alteration of shape, with water having low viscosity and molassis having high viscosity), and (5) cellularity (the number of cells seen under a microscope at a high power of magnification). Women who check their own cervical mucus to determine the pre-ovulation period often assess the mucus collected in terms of amount (similar to volume, usually described as a little or a lot), stretchy-ness (similar to spinnbarkeit, often mucus is pulled between the thumb and forefinger), and clarity (similar to cellularity, often described as ideally similar in appearance to egg white). Immediately prior to ovulation, cervical mucus changes (physically) to facilitate sperm transport. One such change appears to involve the mucin threads that help to form the mucus, such that immediately prior to ovulation these threads form longitudinal pseudochannels to allow sperm to progressively move across the mucus. At any other time during the cycle, the mucin threads are tangled together to restrict the progressive movement of sperm.
| |||||||||||||||